
Our Services
Comprehensive Diagnostic Psychiatry Services
Systematic root-cause investigation identifies the underlying medical factors that limit mental clarity, energy, and mood.
Our Approach
Diagnostic Psychiatry
Systematic root-cause investigation identifies the underlying medical factors—thyroid function, nutritional status, sleep quality, hormones—that limit mental clarity, energy, and mood.
Whether you're struggling with treatment-resistant symptoms or seeking to optimize from 'functional' to 'exceptional,' comprehensive medical-psychiatric assessment changes outcomes.
Most patients achieve significant lasting improvement within 2-3 months through root-cause investigation.
At a Glance
- 75-90 minute initial evaluations
- Comprehensive medical workup
- Most insurance accepted
- Telehealth available
- Serving CA & AZ
- Typical Stabilization: 2-3 months
- Long-term Care: Quarterly 15-30 min visits
- Improvement Rate: 78% sustained outcomes
- Locations: San Francisco, Los Angeles & Phoenix
Clinical Areas
Core Services & Clinical Areas
Comprehensive diagnostic psychiatry addressing the full spectrum of mental health needs
Comprehensive Medical-Psychiatric Assessment
Systematic 16-system investigation and 75-90 minute initial evaluation. We look at the whole picture.
Psychiatric Symptoms Not Improving
When standard treatment isn't working, we look deeper. We investigate underlying medical causes that may be mimicking or worsening psychiatric symptoms.
Perimenopause & Women's Hormonal Health
Investigating hormonal changes that affect mood, anxiety, and cognition. We don't just treat the symptom; we look at the hormonal context.
Men's Hormonal Health & Low Testosterone
Testosterone optimization can have profound effects on mood, energy, and focus. We assess and treat low testosterone as a potential root cause.
PTSD & Trauma-Related Symptoms
Trauma affects the body. We explore medical factors that may be hindering trauma recovery, such as inflammation or sleep disorders.
Insomnia & Sleep Disorders
Root-cause investigation of sleep problems. Sleep is foundational to mental health. We check for apnea, circadian issues, and more.
Comprehensive Medication Management
Evidence-based psychiatric prescribing with strict medical oversight. We optimize your regimen to minimize side effects and maximize efficacy.
Medical Optimization for Plateaued Patients
For those who are 'doing okay' but not 'feeling great.' We look for the fine-tuning opportunities that take you to the next level.
Professional Optimization
Aims to improve functioning from 70-80% to 95-100%. Ideal for executives, professionals, and high-performers.
Executive Burnout & Fatigue
Medical investigation of performance decline. Is it just stress, or is something physiological draining your reserves?
Second Opinions & Diagnostic Clarity
Fresh perspectives on unclear diagnoses. If you've been given multiple labels without a clear path forward, we can help.
Pre-Surgical Psychiatric Clearance
Expert evaluations for surgical candidates (e.g., bariatric, transplant, spinal cord stimulator).
Treatment Approach
The Three-Phase Treatment Model
A structured path from diagnosis to long-term wellness
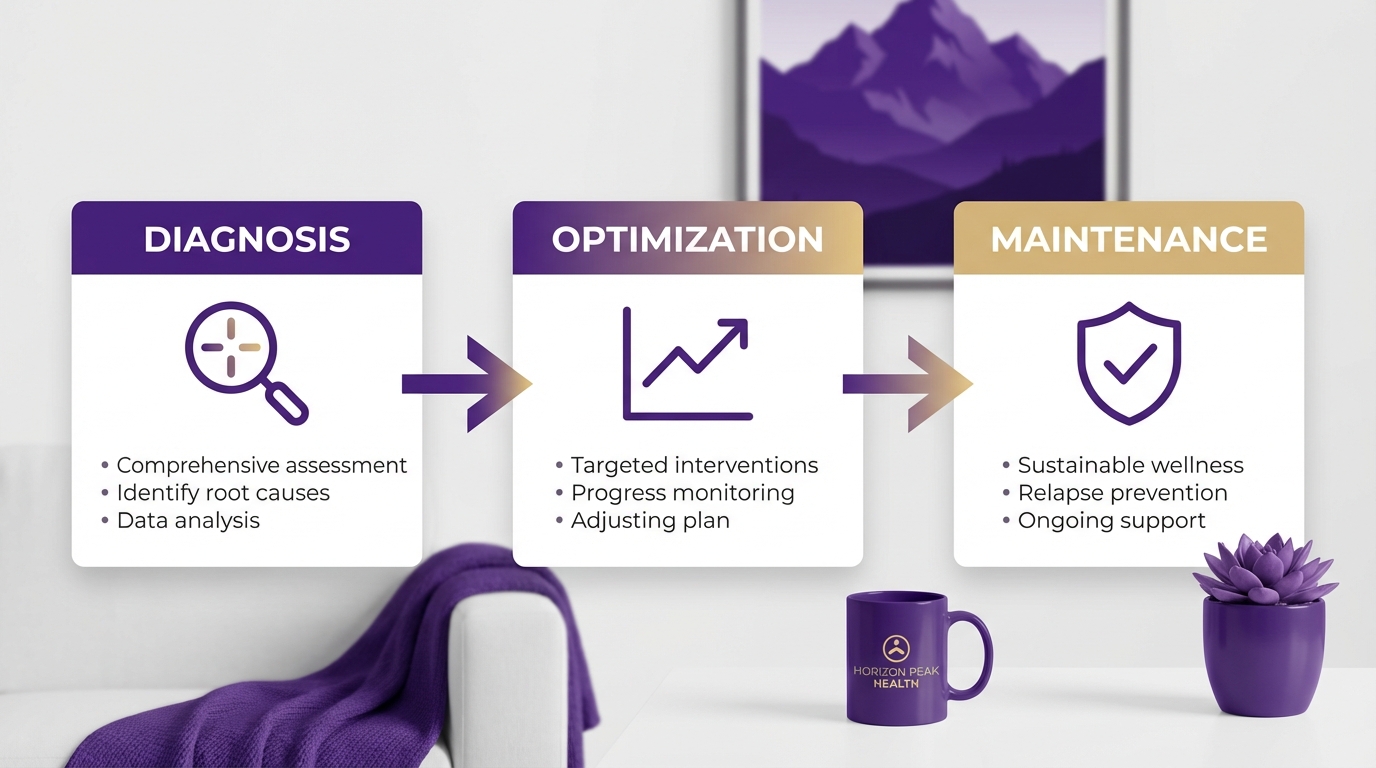
Intensive Diagnosis
Months 1-3
We identify the root causes and start targeted treatment. Frequent adjustments and close monitoring.
Optimization
Months 4-6
Fine-tuning the plan. Symptoms are largely resolved; we focus on full restoration of function and resilience.
Maintenance
Month 7+
Long-term wellness. Simple quarterly check-ins to ensure you stay on track.
Our Locations
Serving Arizona & California
In-person appointments at our Arizona and California locations, plus telehealth available statewide
Chandler, AZ
Serving Chandler, Gilbert, Mesa, Tempe & East Valley
Phoenix, AZ
Serving North Phoenix, Scottsdale, Paradise Valley & surrounding areas
San Francisco, CA
Serving San Francisco, the Peninsula, East Bay & broader Bay Area
Rancho Palos Verdes, CA
Serving the South Bay, Palos Verdes Peninsula & LA County
Torrance, CA
Serving Torrance, Redondo Beach, Gardena & South Bay communities
Long Beach, CA
Serving Long Beach, Lakewood, Signal Hill & LA County
Telehealth appointments available for California and Arizona residents
Experience Diagnostic Psychiatry
Available within 3-5 days. Most major insurance accepted.
Check Availability